Effects of Drinking When You Have an Autoimmune Disease
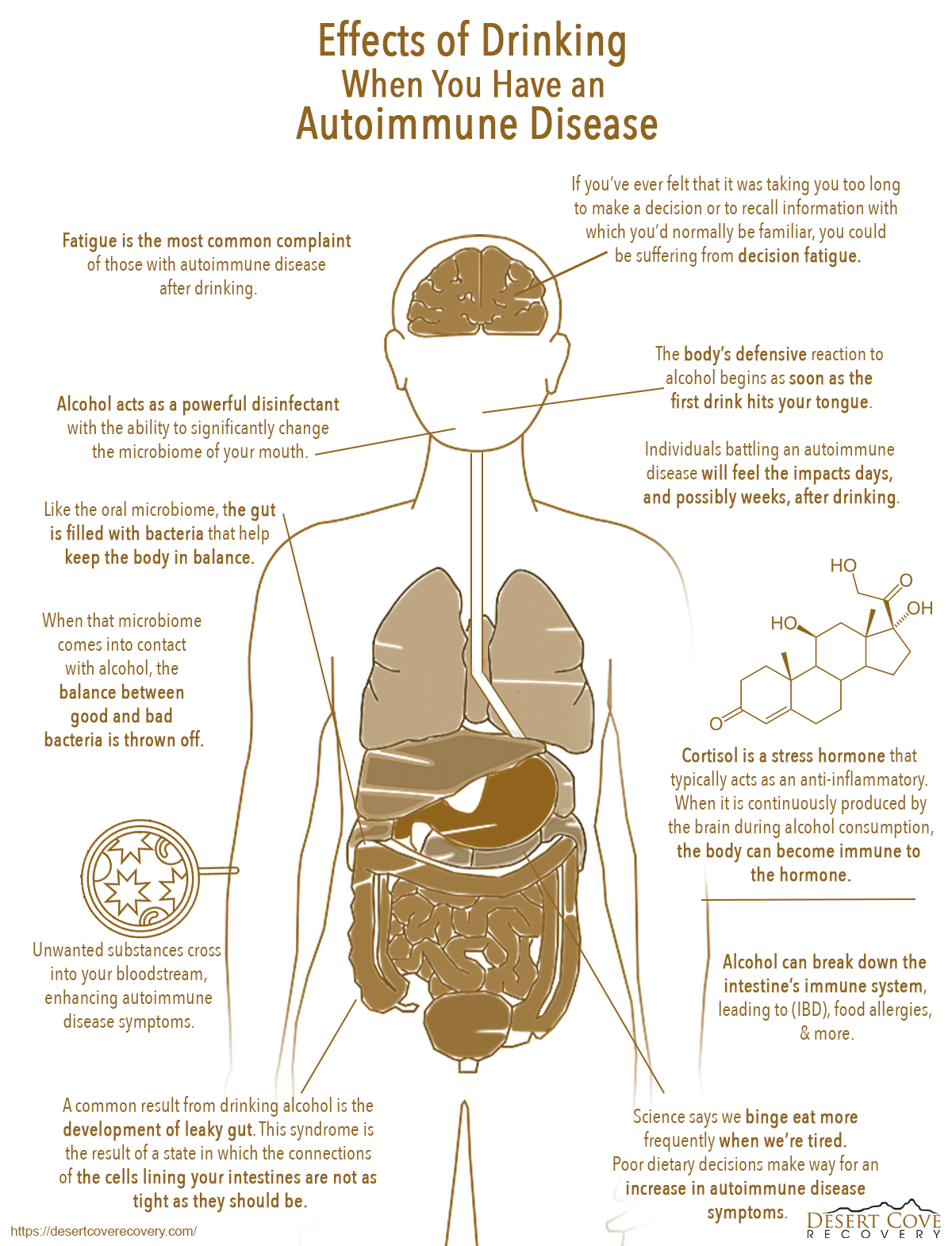
The body’s defensive reaction to alcohol begins as soon as the first drink hits your tongue. While alcohol lowers our defenses and is strongly tied to relaxation in our society, it can wreak havoc on the body’s functionality. Even a person with a healthy immune system can’t escape the effects of drinking, but the effects of drinking with autoimmune diseases can be much more severe.
Continue after video
Alcohol & the Biome
Alcohol acts as a powerful disinfectant with the ability to significantly change the microbiome of your mouth. Like the oral microbiome, the gut is filled with bacteria that help keep the body in balance. When that microbiome comes into contact with alcohol, the balance between good and bad bacteria is thrown off.
The gut, however, may take the hardest hit from the effects of drinking. Alcohol can break down the intestine’s immune system, leading to inflammatory bowel disease (IBD), food allergies, and more.
Based on the detrimental effects of drinking on the body, you may assume we’re referencing a case of alcohol dependency or speaking on data from alcohol rehabilitation Arizona facilities. However, research shows even a moderate or casual amount of alcohol – one to two drinks – can heavily impact someone with an autoimmune disease.
What Is Autoimmune Disease?
Your immune system is made up of cells and organs that protect your body from viruses, bacteria, parasites, and cancer cells. An autoimmune disease causes those cells and organs to attack your body accidentally.
There are more than 100 autoimmune diseases, including:
- Lupus
- Celiac disease
- Ulcerative colitis
- Rheumatoid arthritis
- Multiple sclerosis
- Vasculitis
The National Institutes of Health estimates up to 23.5 million Americans[1], or roughly 7 percent of the population, suffer from autoimmune disease. Of those who are diagnosed with such a disease, 80 percent are women.[2]
The reasons people develop autoimmune diseases are not always clear, but some factors can put you at risk of developing these conditions.
DNA plays a significant role in deciding who suffers from an autoimmune deficiency. Roughly one-third of the risk[3] of developing such a disease is hereditary. It’s also possible “that autoimmune disease occurs based on the immune system’s ability to handle stress,” according to Ana-Maria Orbai, M.D., M.H.S., a rheumatologist at the Johns Hopkins Arthritis Center.[4]
Infections can sometimes lead to autoimmune diseases, and even medications can confuse the immune system and lead it to attack healthy cells. There can also be environmental factors that make it more likely for you to develop these issues. Exposure to mercury, cigarette smoke, and even excess sunlight can all play a role.
Effects Of Drinking On Autoimmune Disease
The effects of alcohol on those with autoimmune diseases have the potential to be much more significant. One can experience an enhanced vulnerability to sickness or feeling sluggish for up to two weeks afterward.
“Physicians have long observed that excessive alcohol consumption can lead not only to liver damage but also to increased illness and death from infectious diseases such as pneumonia,” according to a report[5] from the National Institute on Alcohol Abuse and Alcoholism.
Alcohol rehabilitation in Arizona has found a common result of drinking alcohol is the development of a leaky gut. This syndrome is the result of a state in which the connections of the cells lining your intestines are not as tight as they should be. Unwanted substances cross into your bloodstream, enhancing autoimmune disease symptoms. In addition, autoimmune disease and alcohol feed off one another.
Fatigue
Fatigue is the most common complaint of those with autoimmune disease after drinking. That fatigue, however, can play into other choices that affect the body. Science says we binge eat more frequently when we’re tired.
Our bodies naturally crave sugars and carbohydrates as they desire a quick source of energy. Poor dietary decisions make way for an increase in autoimmune disease symptoms, including inflammation.
In addition, fatigue can make us less intelligent. Suppose you’ve ever felt that it was taking you too long to make a decision or to recall information with which you’d typically be familiar. In that case, you could be suffering from decision fatigue.[6]
When the brain is tired, it conserves energy by making impulse decisions.
Finally, the choices made while fatigued from alcohol consumption when you suffer from an autoimmune disease can lead to weight gain.
Research shows you’re more likely to make poor food choices and skip any exercise, and joint pain can increase. As you become more sedentary, the weight can make autoimmune symptoms more prominent.
Continued after infographic:
Inflammation
Consuming alcohol can cause inflammation. This occurs because the process of breaking down alcohol creates certain compounds that trigger an inflammatory response. One of the most harmful toxins that the process creates is acetaldehyde, but there are many others, including chemokines, cytokines, and more.[7]
Heavy drinking and the inflammation it causes may worsen autoimmune symptoms and, in some instances, may even trigger the disease in someone with a genetic predisposition. Keep in mind that although all alcohol options can lead to inflammation, those that contain significant quantities of sugar are the worst offenders.
Interactions With Autoimmune Disease Medications
Alcohol can also have unpredictable health effects if you’re on certain types of medications for the treatment of autoimmune diseases. Whether you binge drink or have the occasional beer, mixing medications with alcohol is potentially dangerous.
This is especially important for people who take medications to treat type 1 diabetes, rheumatoid arthritis, and lupus.
Methotrexate is a common medication option for those with rheumatoid arthritis, for example, and mixing it with alcohol can increase your chances of developing liver damage.[8]
You also need to be careful if you deal with autoimmune disease flare-ups by taking over-the-counter pain relievers. Drinking alcohol, together with these kinds of anti-inflammatory medications, may increase the risk of bleeding in your gastrointestinal tract.
High Blood Pressure
Another of the most serious ways alcohol can affect your body if you have an autoimmune disease is by making hypertension worse.
Scientists have spotted a link between patients who have high blood pressure and those who develop autoimmune diseases.[9] Autoimmune conditions themselves can cause a spike in blood pressure. If you add alcohol into the mix, you can face serious health issues.
High blood pressure may affect your blood vessels and arteries, making them less elastic. This decreases the flow of oxygen and blood to your heart, putting you at risk of experiencing heart disease. You can have issues like angina, which is heart pain, and heart attacks.
High blood pressure also puts you at risk of experiencing strokes, which occur when part of the brain doesn’t get enough oxygen or if there’s bleeding in or around the brain. Blood vessels that are damaged by high blood pressure can break and leak, and hypertension can also cause blood clots to form, potentially blocking blood flow.
Another danger of high blood pressure is kidney damage. For kidneys to be able to function correctly and filter fluid and waste from your blood, they require healthy blood vessels. High blood pressure may damage blood vessels and put an added strain on the kidneys. This is a particular worry for people with autoimmune diseases like type 1 diabetes.
High blood pressure is one of the most common causes of kidney failure.
Desert Cove Recovery: Trusting an Alcohol Rehabilitation Arizona Facility
If you live with an autoimmune disease, drinking alcohol can be an added stress that your body doesn’t need. If you find yourself struggling to quit drinking alcohol, we can help.
Understanding how to manage your alcohol rehabilitation treatment when you suffer from an autoimmune disease is a specialty of Desert Cove Recovery, allowing us to tailor your treatment to suit your exact needs.
Our drug treatment specialists are highly skilled in dual diagnosis, so we can guide you through any mental health challenges that have developed as a result of pain or living with an autoimmune disease. The caring staff at Desert Cove Recovery is ready to help you overcome alcohol use or dependency so that you can lead a healthier and happier life.
Don’t wait to get the help you need if you’re dealing with an alcohol use disorder. Contact our team today to develop your personalized treatment plan.
To Be Honest with Yourself
However, even when you do not suffer from an autoimmune disease, you should familiarize yourself with alcohol’s effects on the body. Alcohol can cause your heart to become weak, develop a stroke, liver fibroids, mood swings, and high blood pressure, to mention a few.
Once you are familiar with the effects of alcohol on the body, you should self-analyze to determine whether you have a drinking problem. A promising sign that you have an addiction is when you cannot appear in public if you have not sipped your favorite drink. Therefore, you should also take the bold step and enroll in Desert Cove Recovery to avoid your body’s alcohol effects.
Sources:
[1] https://www.gene.com/stories/autoimmune-disease-101 [2] https://www.hopkinsmedicine.org/health/wellness-and-prevention/autoimmune-disease-why-is-my-immune-system-attacking-itself [3] https://www.gene.com/stories/autoimmune-disease-101 [4] https://www.hopkinsmedicine.org/health/wellness-and-prevention/autoimmune-disease-why-is-my-immune-system-attacking-itself [5] https://pubs.niaaa.nih.gov/publications/10report/chap04b.pdf [6] https://blog.trello.com/beat-decision-fatigue-with-better-brain-habits [7] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9966185/ [8] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5561375/ [9] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6394456/
Original blog posed on March 20, 2020. Updated on Feb 29, 2024.